Connect with us
Published
11 years agoon
By
Children, just like adults, are born with essential fungi and bacteria within their bodies considered harmless but can still cause disease under certain conditions. For example, the fungi combine with good bacteria in the digestive tract to maintain optimum functioning of the digestive system.
However, there are times when this delicate balance can be broken, leading to complications such as thrush. Thrush or candidiasis is caused by the overgrowth of the candida albicans fungus.
The fungus is present in the mouth but when the body’s immunity is weakened due to an infection or processes such as chemotherapy, part of the good bacteria is killed, leading to an overgrowth of the fungus and vulnerability of the body to other attacks by harmful bacteria and viruses. Thrush is most common in babies, especially those who are six months and below as their immunity is still weak.
There are other ways, however, of spreading the infection: A mother who is suffering from a yeast infection can pass it to her baby through breastfeeding and on the same token, a child suffering from oral thrush can infect the mother.
Signs that the baby has infected a mother include pain while breastfeeding, which may continue even after the feed is finished, cracked, flaky or sensitive nipples, changes in the colour of nipples or areolas.
Thrush can also be picked when a baby passes through the mother’s infected birth canal. Use of antibiotics or steroid medicines by either the child or breastfeeding mother can also lead to the death of the ‘good’ bacteria leading to overgrowth of the fungus.
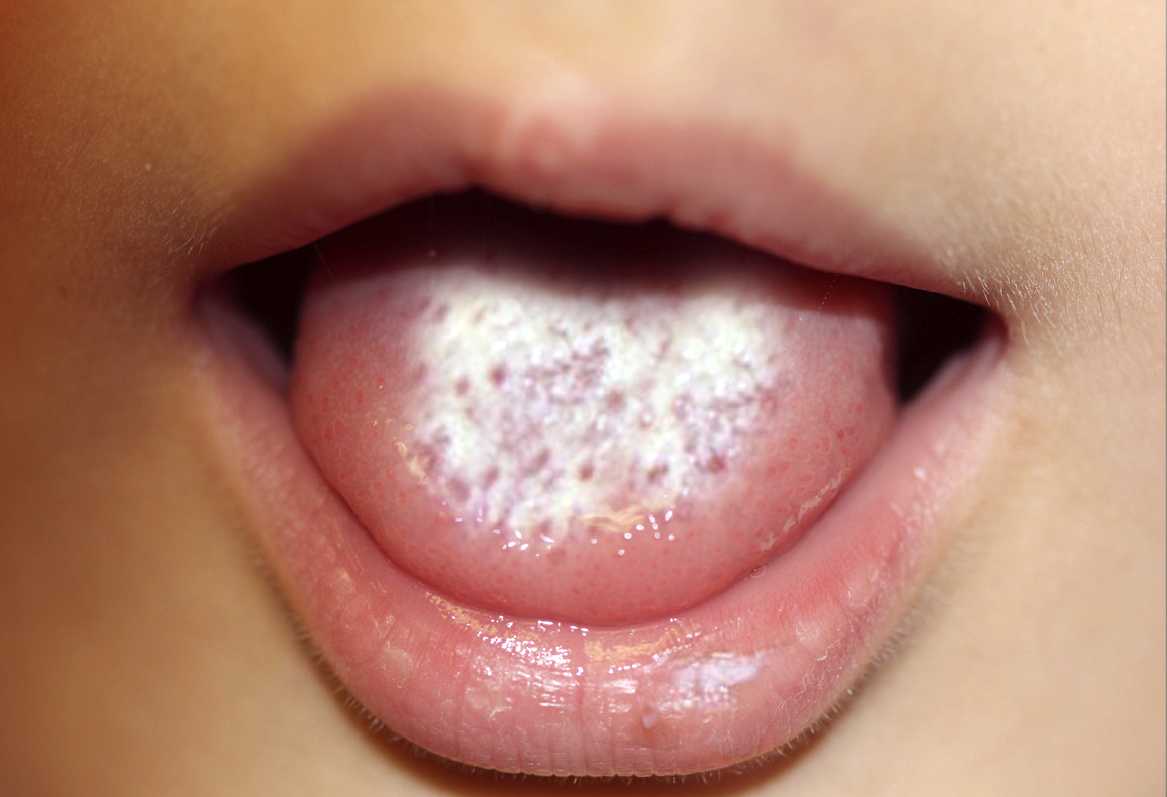
A white patch in your child’s mouth, tongue or lips, which looks like curd and cannot be rubbed off easily, is the most common pointer that your child is suffering from oral thrush.
Milk can also leave a white coating on a baby’s tongue, so ensure you note the difference before jumping into any conclusion. There may also be cracked skin on the corners of the baby’s mouth.
Additionally, irritated, moist skin areas are good breeding grounds for the fungus hence a diaper rash which is fiery red in colour with some areas having a raised red border may mean a thrush infection.
Treatment of thrush
While it can be potentially harmless, the infection can be irritating causing discomfort or pain during suckling or swallowing food, or in the event of a diaper rash.
Some cases go away on their own within a week or two without medical treatment but in case of a severe infection, a doctor will prescribe anti-fungal medicine.
In the event of infection from child to mother, a doctor will prescribe antifungal tablets or cream to apply on the nipples. Do not attempt to scrape off the white patches as this can lead to unnecessary bleeding.
Changing diapers often can also help prevent thrush in the buttocks and thigh area. Keep the skin clean using water, mild soap and pat it dry. Use barrier creams and high absorbency diapers to keep the rash in check.
Remember to wash your hands thoroughly before and after nursing and after each diaper change. A balanced diet can also help keep things in check.
Regular intake of yoghurt rich in lactobacilli bacteria, which are the ‘good’ bacteria, will help the body to regain its equilibrium and remain at its optimum levels.
Ensure that baby’s utensils and toys are sterilised regularly. Use hot water to cleanse bottle teats or pacifiers as it destroys breeding grounds for the fungus as well as preventing re-infection through frequent use.
Storing milk and prepared bottles in the refrigerator also prevents yeast from growing. If your child keeps getting oral thrush, especially after the nine-month mark, consult your doctor as it may be a sign of a different infection altogether.
If treatment has not fully cleared the thrush after a week of treatment, speak to your doctor.
Published in August 2015.



