Editorial
SYSTEMIC LUPUS Understanding this chronic autoimmune disease
At the moment, there is no cure for lupus but there are treatments that can mitigate the symptoms
At the moment, there is no cure for lupus but there are treatments that can mitigate the symptoms
Published
10 years agoon
By
Diana Rachel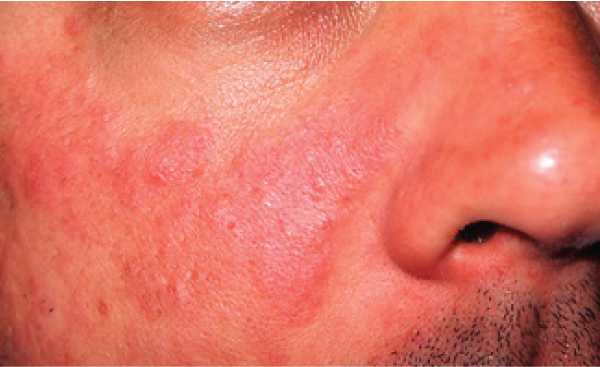
Lupus is one of the most complex conditions and as a result, poorly understood. This may be because it affects many parts of the body. It’s symptoms range from mild to life threatening. The term “lupus” is often used to describe a more severe form of the condition called systemic lupus erythematosus (SLE), which can affect many parts of the body, including the skin, joints and internal organs.
You have probably heard about the idiomatic expression “Frankenstein’s monster.” The phrase is derived from the novel Frankenstein by Mary Shelly in which the protagonist invents a monster that later comes to destroy him. A Frankenstein monster is thus something that cannot be controlled and attacks or destroys the person who invented it. And this description pretty much summarises what lupus is.
Lupus is a chronic inflammatory disease that occurs when your body’s immune system attacks your own tissues and organs. In lupus, something goes wrong with your immune system, which is the part of the body that fights off viruses, bacteria, and germs. Normally, the immune system produces proteins called antibodies that protect the body from these invaders. Autoimmune means your immune system cannot tell the difference between these foreign invaders and your body’s healthy tissues, and creates autoantibodies that attack and destroy healthy tissues.
These autoantibodies cause inflammation, pain and damage. The inflammation caused by lupus can affect many different body systems including your joints, skin, kidneys, blood cells, brain, heart and lungs.
Types of lupus
There are several types of lupus that affect the body differently. These include:
Systemic lupus erythematosus: Systemic lupus is the most common form of lupus and it was what often people mean when they talk about “lupus.” It can affect the kidney (lupus nephritis – it can be so damaging that dialysis or kidney transplant may be needed); the lungs where there would be an increase in blood pressure causing difficulty in breathing; the nervous system or brain leading to headaches, confusion, memory loss and strokes; and the arteries which can lead to a heart attack caused by the build up deposits on the coronary artery walls.
Chronic cutaneous lupus erythematosus: Lupus that is limited to the skin. A skin biopsy is usually obtained to diagnose skin lupus.
Drug-induced lupus erythmatosus: Certain drugs can actually cause lupus-like symptoms in people who do not have SLE. Nevertheless, this form of lupus is temporary and usually subsides within months of the time medication is stopped.
Neo-natal lupus erythmatosus: This form of lupus may affect the babies of women with certain autoantibodies, namely anti-Ro, anti- La, and anti-RNP. In most cases, it affects the baby’s skin and it goes on its own, even without treatment.
Childhood lupus: This lupus occurs in children and it affects the body the same way as adult lupus. It affects certain organs such as the kidneys.
What causes lupus?
It is not exactly clear why the antibodies released by the immune system attack the healthy tissues, organs and cells. However, there have been suggestions that there may be genetic factors that make some people more susceptible to the condition, or environmental factors that may trigger lupus in those who are susceptible.
The environmental factors that may be responsible for triggering lupus include exposure to sunlight and more specifically ultraviolet light, hormonal changes that occur during a woman’s lifetime, certain infections and smoking.
Signs and symptoms of lupus
It is difficult to diagnose lupus since its signs and symptoms often imitate those of other ailments. However, the most idiosyncratic sign of lupus is a facial rash that looks like the wings of a butterfly unfolding across both cheeks. It is noteworthy that this occurs in many but not all cases of lupus. The signs and symptoms largely depend on which body system has been affected by lupus, but the following are the most common signs and symptoms: fatigue and fever, joint pain, stiffness and swelling, butterfly-shaped rash on the face, skin lesions, shortness of breath, chest pain, dry eyes and headache.
Treating lupus
At the moment, there is no cure for lupus but there are treatments that can mitigate the symptoms. This notwithstanding, treatment will in most cases involve a combination of medication and self-care measures. For example, protect yourself from the sun as exposure to sunlight can make symptoms such as rashes worse. One can also take non- steroidal anti-inflammatory drugs (NSAIDs) that reduce inflammation of the body. Some NSAIDs are available over the counter and they include ibuprofen and diclofenac. Hydroxychloroquine is a drug that is used in treating malaria but which can also be used to treat some of the symptoms of lupus such as joint and muscle pain, rashes and fatigue.
Other drugs used in treating lupus are corticosteroids that help reduce inflammation quickly. These are only prescribed if the condition is severe. Rituximab is a new type of medication used in people with severe lupus that doesn’t respond to other treatments. Immunosuppressant, a type of medicine that suppresses your immune system, can help improve your symptoms of SLE by limiting the damage your immune system causes when it attacks healthy parts of your body.
Published in January 2015



