Connect with us
Published
2 months agoon
By
Samuel Owino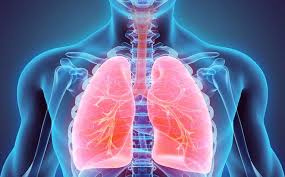
As the world observed World Tuberculosis Day on 24th March 2026, the global fight against one of history’s deadliest infectious diseases stands at a crossroads. While the World Health Organisation (WHO) has unveiled transformative new diagnostic tools, local health systems, particularly in high-burden countries like Kenya, are sounding the alarm over a funding crisis that threatens to allow emerging forms of the disease to spread unchecked.
On March 24, 2026, the WHO issued updated guidelines recommending a suite of innovative diagnostic technologies designed to bring testing closer to the point of care. For decades, the primary hurdle in TB detection has been the reliance on sputum (phlegm) samples, which many patients, especially children and those with advanced HIV, struggle to produce.
The new recommendations introduce tongue swabs as a viable alternative, allowing for easy, non-invasive specimen collection. Furthermore, the WHO is championing near-point-of-care molecular tests that are portable, battery-operated, and can deliver results in less than an hour. These tests are projected to cost half the price of current molecular diagnostics, potentially saving billions in machine time and commodity costs.
“These new tools could be truly transformative,” said Dr Tedros Adhanom Ghebreyesus, WHO Director-General. “By bringing fast, accurate diagnosis closer to people, we can save lives, curb transmission, and reduce costs.”
However, technology alone cannot solve the epidemic if patients remain in the shadows. In Kenya, health officials in Kirinyaga County have flagged a worrying surge in genital tuberculosis, a form of extrapulmonary TB that affects reproductive organs.
Unlike the more common pulmonary TB, which affects the lungs, genital TB is often misdiagnosed due to low awareness and significant social stigma. In women, the bacteria can spread to the uterus, leading to permanent fertility complications if not caught early. Health experts emphasise that while TB is airborne and not a sexually transmitted infection, the stigma surrounding reproductive health often prevents men and women from seeking care.
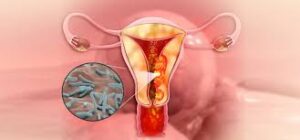
In hotspots like Mwea, officials are now taking screening services directly to markets and social spaces to reach men, who are currently the most affected group due to delayed health-seeking behaviour.
The irony of the 2026 TB response lies in the widening gap between scientific innovation and financial reality. The WHO notes that every dollar invested in TB generates up to $43 in health and economic returns. Yet, global health funding is facing severe cuts.
In Kenya, Members of Parliament recently warned that a funding shortfall, dropping from Kshs 1.3 billion to roughly Kshs 1 billion over the last two years, could reverse decades of progress. These cuts directly impact the rollout of the very technologies the WHO is recommending, such as digital X-rays and the maintenance of GeneXpert machines.
“Every time we reduce funding for these diseases, we risk losing the gains we have made,” warned Patrick Munene, MP for Chuka Igambang’ombe. “Eventually, even the investments already made will go to waste.”
The theme for World TB Day 2026, “Yes! We can end TB: Led by countries, powered by people,” serves as a rallying cry and a warning. Science has provided tools such as tongue swabs for the hard-to-test, portable machines for remote villages, and shorter treatment regimens that have reduced drug-resistant TB therapy from 18 months to just six.
But to bridge the gap between a laboratory breakthrough and a cured patient, the global community must address the funding crisis. Without sustained investment and a concerted effort to dismantle the stigma of silent forms like genital TB, the world’s oldest pandemic may continue to claim many lives every single day.
For more, click HERE to join our WhatsApp channel!





You must be logged in to post a comment Login